What Is HPI in Medical Terms? A Complete Guide to the History of Present Illness

In medical terms, HPI stands for History of Present Illness. It is a detailed, chronological narrative that documents the symptoms, events, and circumstances leading a patient to seek medical attention. As clinicians, we consider the HPI the backbone of the subjective component of a SOAP note (Subjective, Objective, Assessment, Plan). A well-constructed HPI allows the physician to formulate a working differential diagnosis, guide the physical health, and determine an appropriate diagnostic and therapeutic plan.
Simply put, the HPI is where the patient’s story meets clinical reasoning and getting it right is the first step toward accurate patient care.
What Does the HPI Include?
The HPI expands beyond the Chief Complaint (CC) for example, “chest pain” and explores the full clinical picture surrounding the complaint. A thorough HPI should cover the following elements:
- Onset: When the symptom first began.
- Context: What the patient was doing at the time of onset.
- Timing: Whether the symptom is constant, intermittent, progressive, or fluctuating.
- Location: The anatomical site of the symptom.
- Quality: The character of the symptom (e.g., sharp, dull, throbbing, burning).
- Severity: Intensity, often rated on a 0–10 pain scale.
- Modifying Factors: Aggravating and relieving factors.
- Associated Symptoms: Other symptoms accompanying the chief complaint.
- Pertinent Negatives: Symptoms the patient denies that help rule out differential diagnoses.
Each of these components contributes to a clearer clinical picture and supports evidence-based decision-making.
Common HPI Mnemonics (Memory Aids)
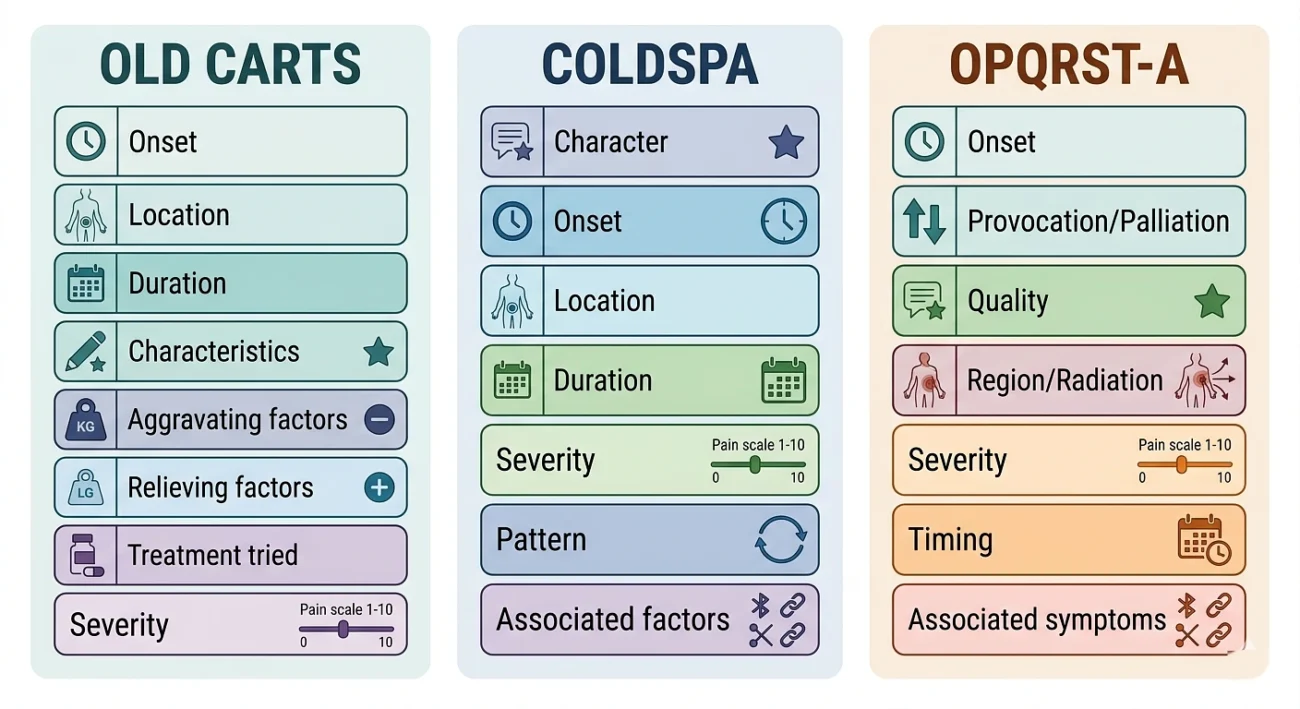
These frameworks serve as a cognitive checklist, particularly valuable for health medicines, residents, and nursing professionals during clinical encounters.
HPI vs. Chief Complaint
Clinicians must distinguish between these two related but distinct elements:
- Chief Complaint (CC): The primary reason for the patient’s visit, usually stated in the patient’s own words (e.g., “headache”).
- HPI: The detailed clinical narrative surrounding that complaint.
Example: “A 30-year-old female presents with a sharp, throbbing headache that began two days ago, localized to the right temple, rated 7/10 in severity, aggravated by light exposure, and partially relieved with acetaminophen.”
This level of detail transforms a one-line complaint into a meaningful clinical story.
How to Document an HPI Correctly
A high-quality HPI should read as a coherent clinical narrative not a bullet-pointed checklist. Follow these documentation principles:
- Begin with a One-Liner: Include basic demographics, relevant past medical history, and the primary complaint. Example: “50-year-old male with a history of hypertension presenting with substernal chest pain.”
- Maintain a Chronological Flow: Describe symptom progression from onset to the time of presentation.
- Use Proper Medical Terminology: Replace lay descriptions with clinical terms (e.g., “productive cough” instead of “coughing up stuff”).
- Include Pertinent Positives and Negatives: Document both present and absent findings relevant to the differential diagnosis.
- Record Prior Interventions: Note any self-medication, over-the-counter treatments, or prior clinical care including response to treatment.
Remember: a well-written HPI tells the patient’s story in a way that any clinician reading it can immediately grasp the clinical context.
Why the HPI Matters in Clinical Practice
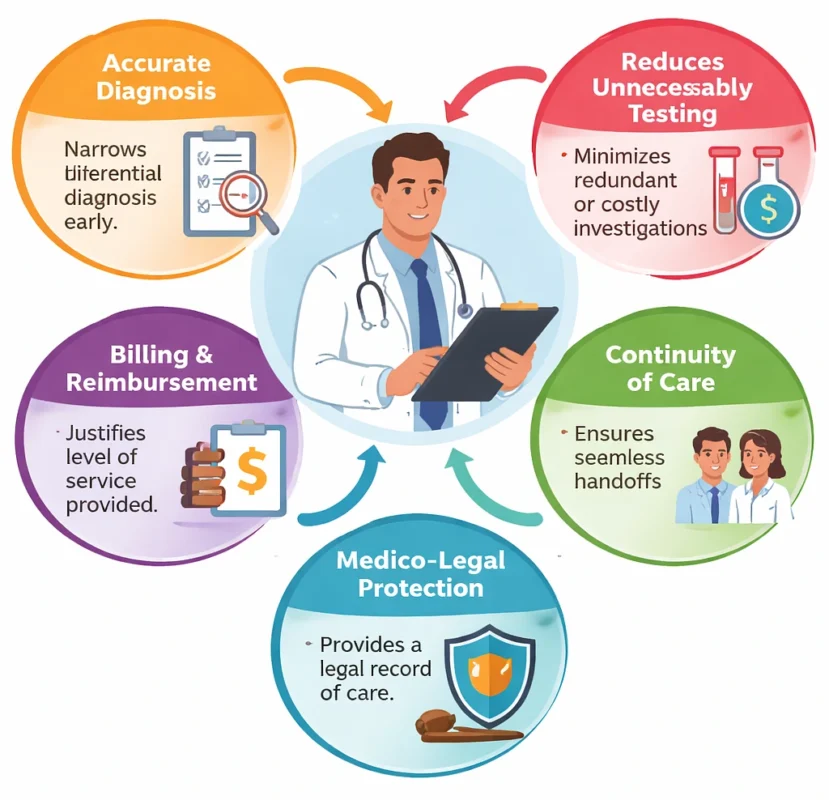
The HPI is not merely a documentation formality it has direct implications for patient outcomes and healthcare delivery:
- Accurate Diagnosis: A comprehensive HPI helps narrow the differential diagnosis early in the clinical encounter.
- Reduces Unnecessary Testing: Thorough history-taking can minimize redundant, invasive, or costly investigations.
- Continuity of Care: A clearly documented HPI ensures that subsequent providers understand the full clinical context without requiring repeat history-taking.
- Medico-Legal Protection: A detailed HPI serves as an essential legal record of clinical reasoning.
- Billing and Reimbursement: Insurance providers often require adequately documented HPIs to justify the level of service provided particularly in complex cases.
Example: A Well-Documented HPI for Chest Pain
“Patient is a 55-year-old male with a known history of hypertension who presents with 2 hours of crushing substernal chest pain. The pain began while mowing the lawn, radiates to the left arm, and is associated with nausea and diaphoresis. He denies shortness of breath, palpitations, or fever. He took one aspirin at home with mild relief. No prior episodes of similar pain.”
This example demonstrates chronological structure, proper terminology, pertinent positives and negatives, and prior intervention all hallmarks of a strong HPI.
Reference
For further reading on documenting the History of Present Illness, visit: – History of Present Illness (HPI)
Additional trusted source: Understanding HPI in Medical Documentation
Disclaimer: This blog is intended for educational and awareness purposes only and should not be considered medical advice. Always consult a licensed healthcare professional for clinical guidance.
