Beyond Chemo: How Advanced Breast Cancer Patients Are Using Immunotherapy in Germany
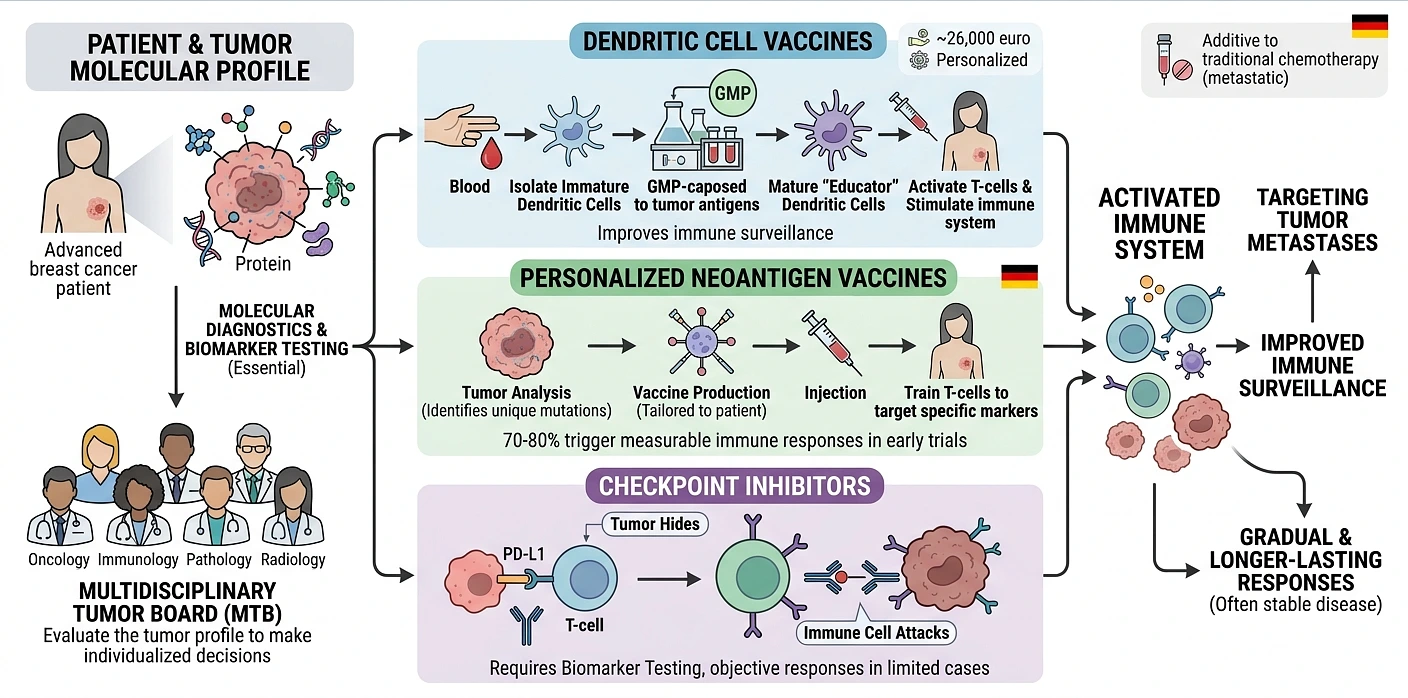
In Germany, more advanced cases of breast cancer patients are also using personalized immunotherapy, including dendritic cell vaccines and checkpoint inhibitors, as an additive to traditional chemotherapy. They are used to treat the metastatic disease and stimulate the immune system to attack the tumors with individualized dendritic cell therapies costing about 26000 euro and concentrating on the improvement of immune surveillance.
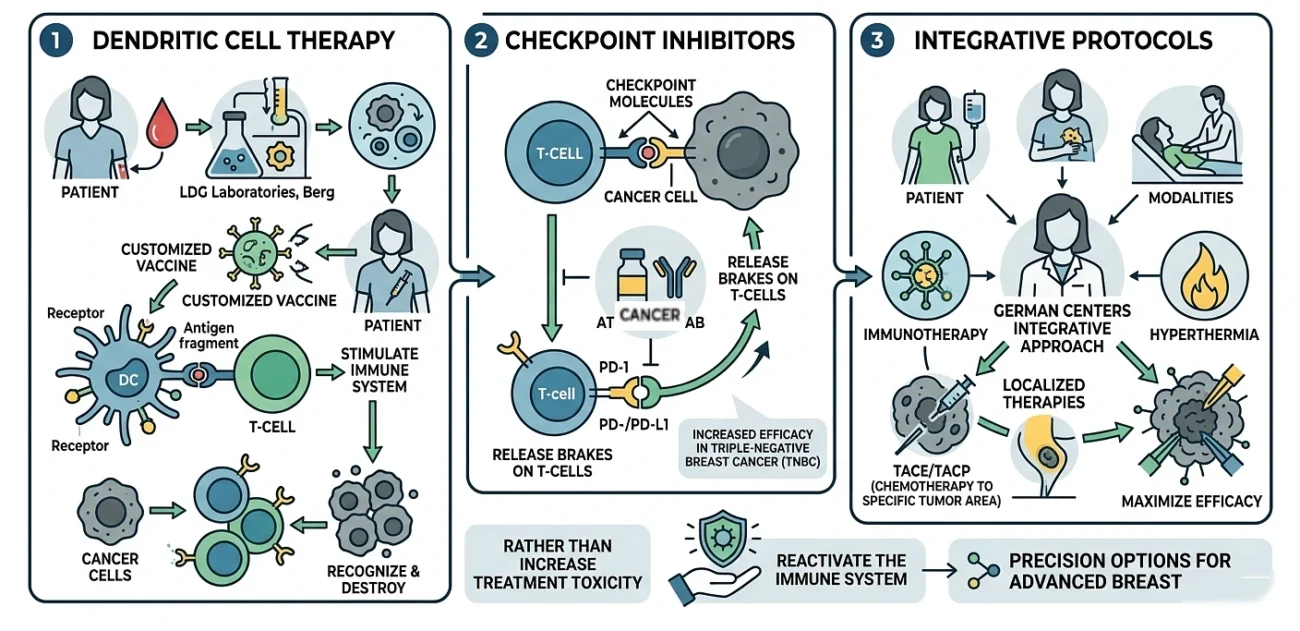
What Expect Breast Cancer Immunotherapy Treatment in Germany
Germany may be considered the nation where numerous patients with advanced breast cancer address their clinics as the ones where modern immunotherapy is incorporated. It is not miracle cures but the everyday care as part of molecular diagnostics and immunology.
Among the greatest advantages, early adoption of new immunotherapies can be noted. Others offer tailor-made vaccinations, dendritic cell-therapy and other immune-modulating therapies that have own GMP-capable laboratory facilities that can produce personalized cellular products.
Tumor biology is also a big concern among the German oncologists. They use mutations, immune, and microenvironmental information to decide whether or not immunotherapy is likely to work. The tumor profile is used to make up treatment plans and not one standard protocol.
- The individual tumor profile of the patient forms the basis of treatment plans and not an individual standard protocol. Discussions are organized in multidisciplinary tumor boards, where the decisions are made with the contribution of oncology, immunology, radiology, and pathology.
Immunotherapy for Breast Cancer: What Patients Need
Immunotherapy has been characterized as a type of treatment which assists the immune system to combat cancer. Nevertheless, it becomes a more apparent concept when you realize that most tumors merely learn to evade immune cells. Immunotherapy aims at restoring the tumor to visibility in order to allow the immune system to react.
All breast cancers do not respond in a similar manner. Some subtypes have properties, like higher mutation load or specific immune markers, which are more apt to be beneficial. Under other conditions, immunotherapy is used to make a complement to the already administered treatments to the patient.
Recent studies indicate that checkpoint inhibitors cause objective responses in less than 10 percent of breast cancer patients in general and that is why biomarker testing is necessary prior to deciding on using this modality.
In Germany, immunotherapy is more widely applied in the clinic since they are more dependent on molecular diagnostics in order to assess the immune profile of the tumor. That allows making a conclusion about whether a patient will respond and which of the immunotherapy, checkpoint inhibitors, cellular therapy, or personalized vaccine will be applicable.
Immunotherapy is not a substitute to any other therapy and it cannot be applied to all. Nevertheless, in the event of a success, the responses can be longer lasting and less toxic than recurrent chemotherapy, so that many patients could regard it as a part of a comprehensive treatment process.
Personalized Breast Cancer Vaccines in Germany
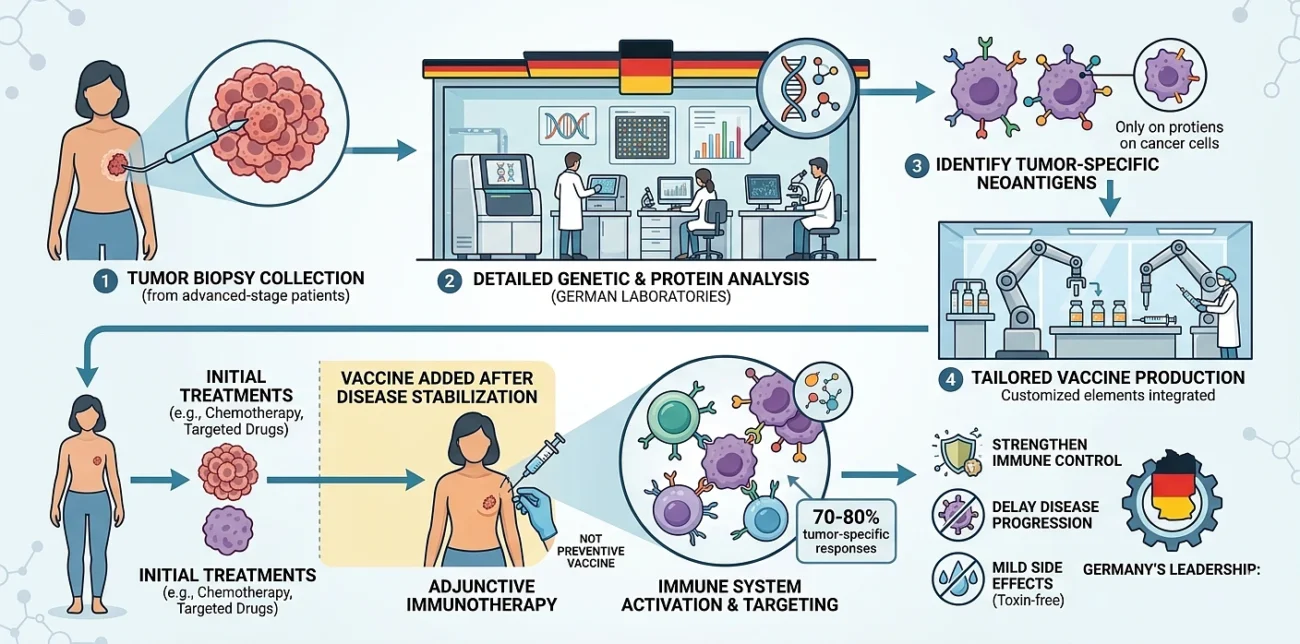
Personalized breast cancer vaccines in Germany are one of the most advanced immunotherapy options. They are not “preventive vaccines,” but treatments tailored to each patient using mutations and proteins found in their own tumor. The goal is to help the immune system recognize these tumor‑specific markers more effectively, especially in patients who have already gone through several lines of therapy.
The analysis of the genetic and protein profile of the tumor begins the process. This information is used by German labs to determine antigens expressed on cancer cells only. A vaccine is then prepared to train the immune system to attack such antigens more precisely.
Early‑phase trials show that personalized neoantigen vaccines trigger measurable tumor‑specific immune responses in about 70–80% of patients.
They are not substitutes to chemotherapy or targeted drugs. They are typically given when the disease has been reduced or stabilized by initial treatments to aid in enhancing immune control and slowing the disease. The side effects are mostly mild since there is no introduction of toxins with the vaccine. It merely directs the immune system.
Germany is the pioneer in this area with the help of clinics with the necessary laboratory capacity and regulatory framework to develop individualized vaccines. To international patients, this implies the availability of a degree of molecular personalization which is still scarce in most countries.
Dendritic Cell Therapy: A Practical Guide for Patients
Dendritic cell therapy is one of the more established personalized immunotherapy options in Germany. Dendritic cells act as the “teachers” of the immune system, showing T‑cells which targets to attack. In many cancers, this process stops working, and the immune system no longer recognizes the tumor.
Treatment begins by collecting a small amount of blood, isolating immature dendritic cells, and exposing them to antigens from the patient’s tumor in a laboratory setting. The prepared cells are then injected back into the patient, usually into the skin or a lymph node area.
The procedure is generally well tolerated. Blood collection is straightforward, and injections cause only mild effects such as low‑grade fever, fatigue, or temporary redness.
Clinical reviews show that dendritic cell vaccines produce objective tumor responses in fewer than 15% of patients but maintain a very favorable safety profile.
A lot of patients have multiple treatment cycles during weeks or months. The goal is not to shrink the tumor fast, but to strengthen the immune surveillance gradually, frequently combined with other interventions that decrease the tumor burden.
Germany has become a leader for this approach thanks to long‑standing experience in cellular immunology and the laboratory capacity needed to produce individualized vaccines. For international patients seeking a clear guide to dendritic cell cancer vaccines, it remains one of the most experienced destinations.
Realistic Expectations: Benefits of Immunotherapy
- Immunotherapy can help some breast cancer patients, but is not effective for everyone response depends on tumor biology and immune system strength.
- Some tumors are easier for immune cells to recognize; others remain almost completely “silent” to the immune system.
- Triple-negative breast cancer (TNBC) tends to show more immune activity, making it a better candidate for checkpoint inhibitors in selected cases.
- Tumors with high mutation burden, mismatch-repair deficiency, or strong inflammatory markers may also respond more sensitively to immunotherapy.
- Hormone-receptor–positive tumors often have a less active immune environment, meaning immunotherapy may only work when combined with treatments that modify the tumor microenvironment.
- German clinics prioritize identifying these biological factors before recommending immunotherapy, rather than applying it broadly.
- Molecular profiling tests help determine whether immunotherapy is likely to be effective, or if a different treatment would be a better fit.
- Even when immunotherapy is suitable, results typically appear slowly the goal is long-term disease stabilization, not rapid tumor shrinkage.
- Outcomes vary: some patients remain stable for extended periods, while others may see little visible change.
- The key principle is matching treatment to tumor biology immunotherapy should not be used simply because other options have been exhausted.
Accessing Cancer Treatment and Immunotherapy in Germany with Aeromedical
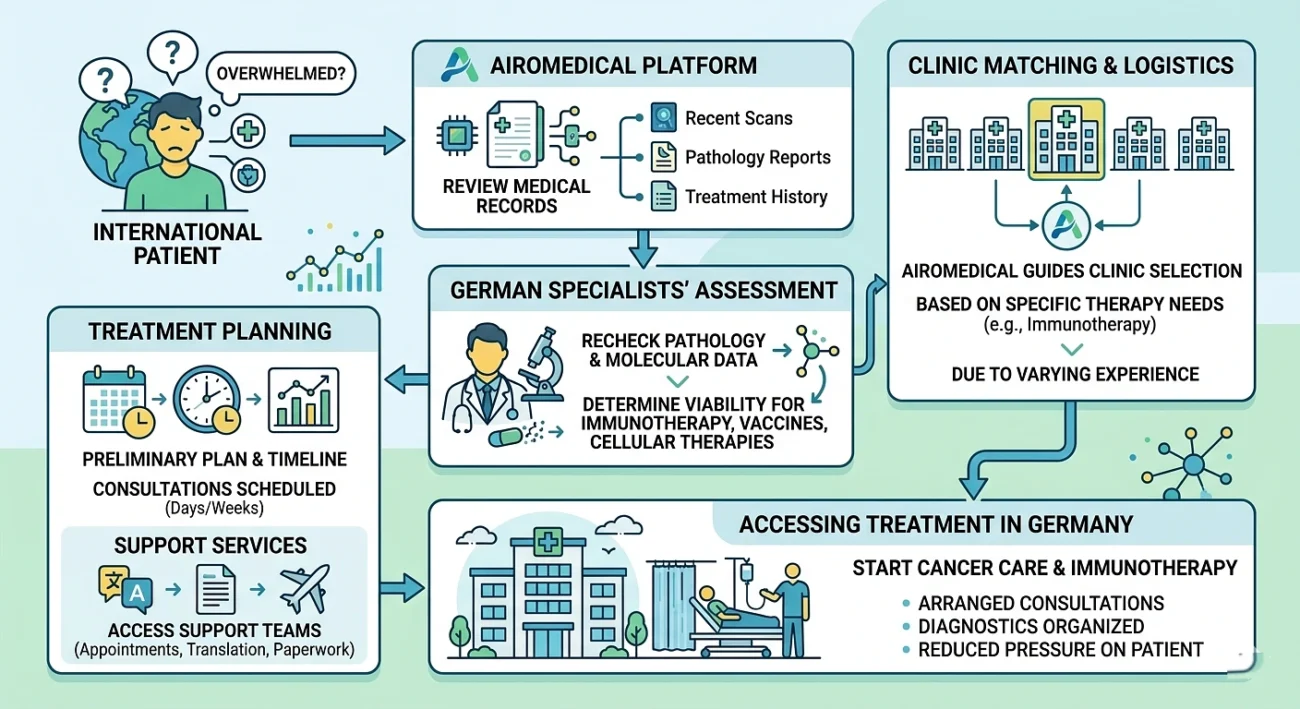
To a lot of foreign patients, it may seem daunting with planning cancer treatment outside their country. Nevertheless, the procedure in Germany is typically not as (apparently) complicated as anticipated. The clinics start by examining the scans, pathology results, and history of treatment of a patient. It demonstrates whether any of the immunotherapy, personalized vaccines, or dendritic cell therapy can be helpful. German experts tend to re-examine the pathology and molecular information in order to have a clear picture before prescribing on how to be treated.
In case of treatment appearing to be necessary, a preliminary plan and schedule is offered at the clinic. The consultations are usually arranged in days or weeks. Travel logistics are manageable with most of the large centers having teams that assist in appointments, translation, and paperwork.
The most difficult is usually the selection of the appropriate clinic. German hospitals are different in terms of experience in the field of immunotherapy and cellular treatments, and thus, it is not always easy to select a clinic. Airemedical platform assists by examining medical history and sending patients to the centers that really offer the therapies they require. Once a clinic is selected, the team assists in making an appointment and relevant diagnostics, which relieves much of the burden of planning care in a foreign country.
References
- Emens L.A., Adams S., et al. Immune checkpoint inhibitors in breast cancer: updated clinical response patterns and biomarker insights. Journal for ImmunoTherapy of Cancer, 2025.
- Dr. Ahmed F. & Dr. Marta Volvak. Dendritic Cell Therapy for Breast Cancer in Germany. Airomedical, 2026.
- Sahin U., Miller M., et al. Personalized RNA mutanome vaccines mobilize poly‑specific therapeutic immunity against cancer. Nature, 2021.
- Kozina J. & Dr. Volvak A. Dendritic Cell Cancer Therapy Guide. Airomedical, 2025.
- Ott P.A., Hu Z., Keskin D.B., et al. An immunogenic personal neoantigen vaccine for patients with melanoma and solid tumors. Nature, 2023.
- Kreiter S., Vormehr M., van de Roemer N., et al. (2024). Neoantigen vaccine–induced T‑cell responses: a systematic review of early‑phase clinical trials. Cancers (MDPI), 2024.
