Tibia (Shin Bone): Location, Anatomy, and Common Conditions
You’ve probably bumped your shin against a coffee table at least once. That sharp, eye-watering pain? You can thank your tibia for that unforgettable moment.
The tibia, commonly known as the shin bone, plays a huge role in how your body moves. Yet most people don’t think about it until something goes wrong.
Whether you’re dealing with shin pain after a run, recovering from an injury, or just want to understand how your body works this guide has you covered. We’ll walk through where the tibia sits, how it’s built, what it does, and the problems that commonly affect it.
You’ll also learn things most guides skip. Like how the tibia develops during childhood, how doctors use it in emergencies to save lives, and what compartment syndrome actually means.
Where Is the Tibia?
The tibia is the larger of the two bones in your lower leg. It sits on the inner side, which doctors call the medial side.
Try running your hand down the front of your leg between your knee and ankle. That hard ridge you feel right under the skin that’s your tibia. Very little muscle or fat covers the front of it, and that’s exactly why banging your shin hurts so badly.
Your tibia stretches from just below the knee joint all the way down to the ankle. At the top, it meets the femur (thigh bone) to form the knee. At the bottom, it connects with the talus bone in your foot to form the ankle.
On the outer side of your leg, you’ll find the fibula a thinner bone that connects to the tibia at both ends. A tough sheet of tissue called the interosseous membrane holds the two bones together along their length.
As for size, the tibia ranks as the second longest bone in the human body, right after the femur. In most adults, it measures around 36 cm roughly 14 to 15 inches long.
Here’s a fun fact: the word “tibia” comes from Latin and originally meant a type of flute. People in ancient times sometimes carved flutes from the tibial bones of animals!
Detailed Anatomy of the Tibia
Like other long bones, the tibia breaks down into three main sections:
- Proximal end (top)
- Shaft (middle)
- Distal end (bottom)
The Proximal End (Top of the Tibia):
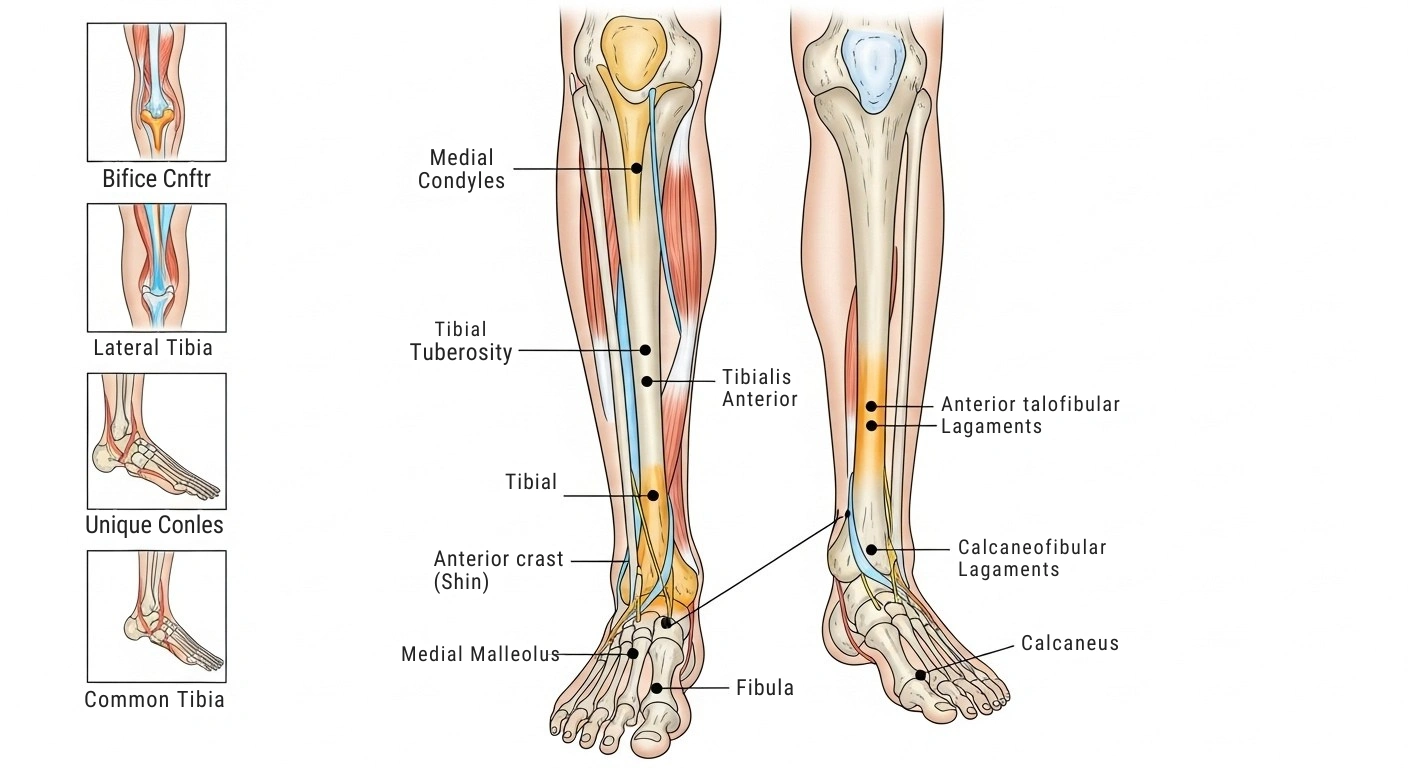
The top part is the widest. It flares out and forms two flat platforms the medial condyle and the lateral condyle. The medial one is slightly larger.
Together, these two condyles make up the tibial plateau. This flat surface supports the bottom end of the femur and handles a lot of your body weight. Any damage here can seriously mess up how your knee works.
Sitting between the condyles, you’ll find a raised area called the intercondylar eminence, also known as the tibial spine. It sticks up on either side as the medial and lateral intercondylar tubercles. Some doctors refer to the lateral one as the Gerdy tubercle.
The ACL and PCL two key knee ligaments you’ve probably heard about in sports news attach near this area. The menisci connect here too.
Now, look at the front side just below the condyles. There’s a bump called the tibial tuberosity. You can feel it easily below your kneecap. Your patellar tendon attaches right here, linking your kneecap to your shin bone. This spot works hard every time you straighten your knee walking, jumping, kicking, you name it.
The Shaft (Middle Section):
If you slice the tibial shaft in cross-section, it looks like a triangle. That gives it three borders and three surfaces.
Three Borders:
- Anterior border — the sharp edge running down the front of your shin. It starts at the tibial tuberosity and goes all the way down. This is the part that takes the hit when you walk into furniture.
- Medial border — runs from the back of the medial condyle down to the medial malleolus.
- Lateral border (interosseous crest) — the interosseous membrane attaches along this edge, holding the tibia and fibula together.
Three Surfaces:
- Medial surface — smooth and subcutaneous, meaning it sits right under your skin with almost no muscle on top. You can feel it along the entire length of your leg.
- Lateral surface — muscles from the front compartment of the leg cover this side.
- Posterior surface — features the soleal line, a diagonal ridge where the soleus muscle starts. The flexor digitorum longus and tibialis posterior also begin here.
You’ll also find a small hole on the posterior surface called the nutrient foramen. This is where the tibia’s main blood supply enters the bone. It usually sits just above the soleal line.
The Distal End (Bottom of the Tibia):
The bottom end is smaller than the top, and its shape shifts from triangular to more rectangular.
Here are the key landmarks:
- Medial malleolus — that bony bump on the inside of your ankle. It helps keep your ankle joint stable.
- Fibular notch — a groove on the outer side where the fibula fits snugly against the tibia.
- Inferior articular surface — the smooth bottom that rests on top of the talus bone.
Behind the medial malleolus, there’s a groove. The tibialis posterior tendon runs through it.
Joints and Articulations of the Tibia
A lot of guides only mention two or three joints. But the tibia actually takes part in four:
- Knee joint — the proximal tibia meets the femur here. It’s the largest and most complex joint in your body.
- Superior tibiofibular joint — the proximal tibia meets the fibula head. A small synovial joint that allows slight gliding movement.
- Inferior tibiofibular joint — the fibular notch connects with the distal fibula. Strong ligaments hold this fibrous joint together, and it’s essential for ankle stability.
- Ankle joint (talocrural joint) — the distal tibia and medial malleolus sit on the talus. This hinge joint lets you point your foot up and down.
On top of these four, the interosseous membrane between the tibia and fibula works as a fibrous joint, called a syndesmosis, along the full length of both bones.
Muscles Attached to the Tibia
Your tibia anchors about 11 muscles. Some start from it, and others end on it.
Muscles That Start from the Tibia:
- Tibialis anterior — comes off the lateral surface and lifts your foot upward.
- Extensor digitorum longus — starts at the lateral condyle and straightens your toes.
- Tibialis posterior — originates from the posterior surface and supports the arch of your foot.
- Soleus — begins at the soleal line. It’s a major calf muscle you use for walking and running.
- Flexor digitorum longus — also starts on the posterior surface and curls your toes downward.
Muscles That Attach onto the Tibia:
- Sartorius and gracilis — connect to the medial surface of the proximal tibia.
- Quadriceps femoris — attaches to the tibial tuberosity through the patellar tendon.
- Semimembranosus — connects to the medial condyle.
- Semitendinosus — attaches just below the medial condyle.
- Popliteus — connects along the soleal line on the back surface.
- Tensor fasciae latae — reaches the lateral tubercle through the iliotibial band.
What Does the Tibia Do?
Your tibia handles several important jobs every single day.
It Bears Your Weight:
The tibia carries about 80 to 90 percent of your body weight in the lower leg. The fibula picks up the rest. Every step you take, every jump you make your tibia absorbs and transfers those forces between your knee and ankle.
It Supports Movement:
Think of the tibia as a lever. When your muscles contract, they pull on this bone to make you walk, run, jump, and climb stairs. Without it, your lower leg muscles would have nothing to pull against.
It Forms and Stabilizes Joints:
Since the tibia takes part in four different joints, it plays a big role in keeping your knee steady, your ankle stable, and your whole lower limb properly aligned.
It Stores Bone Marrow:
The shaft holds mostly yellow marrow, which stores fat. The ends contain some red marrow and that red marrow produces red blood cells, white blood cells, and platelets. Pretty important stuff.
Blood Supply and Nerve Supply
The tibia gets its main blood from the nutrient artery, a branch of the posterior tibial artery. This artery enters through the nutrient foramen on the back surface and feeds the inner two-thirds of the bone.
The outer parts and both ends receive blood from periosteal arteries tiny vessels that run along the periosteum, the thin tissue layer wrapping around the bone.
As for nerves, branches of the tibial nerve and the common peroneal (fibular) nerve supply the tibia and its periosteum. That periosteum has a ton of nerve endings, which explains why even a minor shin knock can send you through the roof.
Bone Development and Ossification of the Tibia
Most guides skip this part, but it matters especially if you’re a parent or a young athlete.
Your tibia doesn’t start out as one solid piece of bone. Instead, it develops through a process called endochondral ossification. Basically, a cartilage model slowly turns into real bone over time.
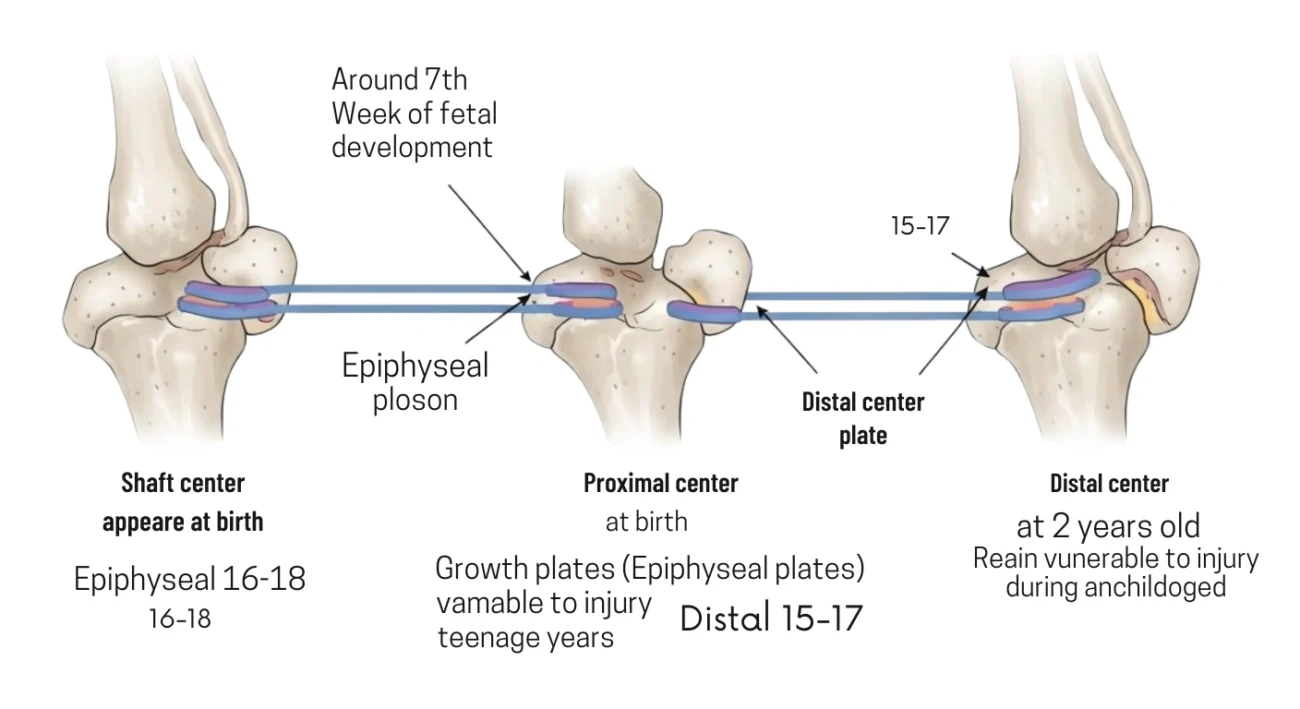
This process kicks off from three separate centers:
- Shaft center — shows up around the 7th week of fetal development.
- Proximal center (top) — appears around the time of birth.
- Distal center (bottom) — appears during the second year of life.
Between these centers sit the growth plates, also called epiphyseal plates. These cartilage zones let the bone grow longer throughout childhood and the teenage years.
The proximal growth plate usually closes around age 16 to 18. The distal one closes around age 15 to 17. Until they close, these areas stay vulnerable to injury. That’s why active kids and teenagers deal with problems like Osgood-Schlatter disease and growth plate fractures more often than adults.
How the Tibia Changes with Aging
Your tibia doesn’t stay the same your whole life. Things change as you get older.
Bone density hits its peak around age 30. After that point, your body breaks down old bone a little faster than it builds new bone. For women, this process speeds up a lot after menopause because estrogen levels drop and estrogen plays a big role in protecting bone health.
Over the years, the cortical bone (the hard outer shell) gets thinner. The trabecular bone (the spongy stuff inside the ends) loses density. All of this makes your tibia more likely to break, even from a minor fall.
The cartilage covering the tibial plateau also wears down with time. That can lead to osteoarthritis in the knee, bringing pain, stiffness, and less mobility.
But here’s the good news. Staying active, eating calcium-rich foods, getting enough vitamin D, and doing weight-bearing exercises throughout your life can slow all of these changes down.
Common Conditions That Affect the Tibia
Tibial Shaft Fractures:
These rank among the most common long bone fractures out there. They usually happen because of high-energy trauma think car accidents, bad falls, or hard sports collisions.
You’ll know something’s wrong because of severe pain, swelling, trouble putting weight on the leg, and sometimes a visible deformity. Doctors treat stable fractures with a cast. If the bone shifts out of place or breaks through the skin, surgery becomes necessary typically an intramedullary nail (a rod inside the bone) or plates and screws.
Tibial Plateau Fractures:
These happen at the very top of the tibia and involve the knee joint surface. They’re common after falls from a height or a direct blow to the side of the knee.
Because the joint surface takes the damage, leaving a plateau fracture untreated can cause arthritis and meniscus problems down the road. Many of these fractures need surgery.
Distal Tibial and Ankle Fractures:
Fractures at the bottom of the tibia often affect the ankle too. Two specific types worth knowing:
- Pilon fracture — damages the distal tibia’s joint surface with the ankle, usually from a high-energy fall.
- Tillaux fracture — affects the growth plate area in teenagers.
Both types typically require surgery to fix properly.
Shin Splints (Medial Tibial Stress Syndrome):
If you’ve ever felt a nagging ache along the inner edge of your shin after running, you’ve probably had shin splints. The pain usually hits the lower two-thirds of the tibia.
What causes it? The muscles, tendons, and periosteum attached to the tibia get irritated. Overtraining, running on hard surfaces, worn-out shoes, and flat feet or high arches all play a part. Rest, ice, better shoes, and a smarter training plan usually do the trick.
Stress Fractures:
These are tiny cracks in the bone that build up over time from repetitive force not from one single hit. Runners, dancers, and military recruits get them a lot.
The main symptom is a dull ache that gets worse during activity and eases up with rest. Regular X-rays often miss stress fractures early on, so doctors typically order an MRI or bone scan to confirm.
Osgood-Schlatter Disease:
This one mainly hits teenagers going through growth spurts especially those who play sports with lots of running and jumping. It causes pain and swelling right at the tibial tuberosity.
What happens is the patellar tendon keeps pulling on the growth plate at the top of the tibia, irritating it. The good news? It usually goes away on its own once the growth plate closes.
Blount Disease:
Blount disease also targets the growth plate at the top of the tibia. When too much weight or mechanical stress pushes on it, the inner part of the plate slows down. But the outer part keeps growing normally. The result? The tibia starts bowing outward instead of growing straight.
This condition shows up in toddlers (infantile form) and sometimes in teenagers too. Mild cases respond to bracing. Severe cases need surgery.
Paget’s Disease of Bone:
With Paget’s disease, abnormal bone remodeling makes bones bigger, weaker, and more likely to break. When it hits the tibia, the bone can bow outward, causing pain and making it tough to walk. Doctors usually treat it with bisphosphonate medications.
Osteoporosis:
Osteoporosis thins out your bones by reducing their density. Since the tibia bears so much weight, it becomes a prime target for fractures sometimes even from a simple stumble. This condition affects older adults most often, especially women after menopause. A DEXA scan can catch it early.
Osteomyelitis:
Osteomyelitis means a bone infection. It most commonly develops after an open fracture or surgery, when bacteria find their way inside. Symptoms include deep pain, swelling, redness, and fever. Treatment usually involves weeks of antibiotics, and severe cases may need surgery to clean out the infected tissue.
Posterior Tibial Tendinitis:
This happens when the tendon running behind your medial malleolus gets irritated or swollen. You’ll feel pain on the inner side of your ankle. If you ignore it long enough, the arch of your foot can start to weaken.
Compartment Syndrome: A Serious Emergency
This condition deserves its own section because it can be life-threatening, and most people have never even heard of it.
Your lower leg contains four compartments. Tough tissue called fascia wraps around each one. Inside, you’ll find muscles, nerves, and blood vessels.
When a tibial fracture or serious injury causes swelling inside one of these compartments, pressure starts building. Since fascia doesn’t stretch much, the pressure has nowhere to escape. Eventually, it can cut off blood flow to the muscles and nerves inside.
Warning signs you should never ignore:
- Severe pain that seems way worse than the injury itself
- Tightness and hard swelling in the leg
- Numbness or tingling in the foot or toes
- Weakness when you try to move your foot
- Pain that spikes when someone gently stretches your toes
The only fix is a fasciotomy a surgery where the surgeon cuts open the fascia to release the pressure. If doctors don’t act within about six to eight hours, the damage can become permanent. We’re talking dead muscle tissue, nerve injury, or in the worst cases, amputation.
If you’ve had a tibial fracture and the pain keeps getting worse instead of better, get to the emergency room right away.
The Tibia in Emergency Medicine: Intraosseous Access
Here’s something almost no anatomy guide mentions: your tibia can literally save your life.
When paramedics or ER doctors can’t get an IV line started during cardiac arrest, severe trauma, or shock, for example they turn to a technique called intraosseous (IO) access. They push a special needle directly into the bone marrow of the tibia.
The two most common IO sites on the tibia:
- Proximal tibia, just below the knee the go-to spot.
- Distal tibia, just above the ankle the backup option.
Why does this work? Because the bone marrow has a dense network of veins that feeds directly into your body’s circulation. Fluids, medications, and even blood products delivered this way reach your heart and organs almost as fast as a regular IV.
IO access has become standard practice in emergency medicine. It has saved countless lives in situations where every second counts.
How Doctors Diagnose Tibia Problems
It all starts with a physical exam. Your doctor will check for swelling, tenderness, any deformity, and how well you can move the leg. They’ll also look for signs of compartment syndrome.
After the exam, imaging usually comes next:
- X-rays — the go-to first step for spotting most fractures and bone problems.
- MRI — the best option for stress fractures and soft tissue injuries that X-rays miss.
- CT scan — helpful for complex fractures, especially tibial plateau breaks, when doctors need to plan surgery.
- Bone scan — picks up infections and metabolic bone diseases like Paget’s.
- DEXA scan — measures bone density and helps diagnose osteoporosis.
Treatment and Rehabilitation
Conservative Treatment:
For milder issues like shin splints and early stress fractures, the plan usually includes rest, ice, anti-inflammatory medications, and a slow return to activity.
Surgical Treatment:
More serious fractures may need one of these approaches:
- Intramedullary nailing — a metal rod goes inside the bone’s canal to hold everything in place.
- Plate and screw fixation — hardware goes on the outside of the bone.
- External fixation — a frame sits outside the leg, connected to the bone through pins.
- Fasciotomy — emergency surgery for compartment syndrome.
Physical Therapy and Rehabilitation:
Rehab plays a critical role in almost every tibia recovery. A good program will focus on:
- Getting your range of motion back in the knee and ankle
- Rebuilding strength in the surrounding muscles
- Improving balance and coordination
- Gradually working your way back to walking, running, and sports
Starting to move early safely and with guidance helps prevent stiffness, muscle loss, and blood clots. Most tibial fractures take anywhere from 12 weeks to 6 months to heal fully, depending on how bad the break was and what treatment you needed.
How to Protect Your Tibia
Taking care of your shin bone isn’t rocket science. A few smart habits make a real difference:
- Wear shoes that fit well and give you proper support, especially when exercising.
- Build up your training gradually don’t suddenly double your running distance overnight.
- Mix up your workouts so you’re not stressing the same bones and muscles every day.
- Eat enough calcium and vitamin D to keep your bones strong throughout life.
- Always warm up before exercise and cool down after.
- If your shins start hurting during activity, stop. Early rest prevents small problems from turning into big ones.
For parents keep an eye on your kids if they complain about leg pain during sports. Catching conditions like Osgood-Schlatter and Blount disease early makes treatment much simpler.
FAQs
Is the tibia the same as the shin bone?
Yes, they’re the same thing. Tibia is just the medical name for the shin bone the bigger bone on the inner side of your lower leg.
Why does hitting your shin hurt so much?
Because there’s almost no muscle or fat protecting the front of the tibia. The periosteum a tissue layer packed with nerve endings sits right under the skin. When you bang your shin, the impact hits those nerves directly.
How long does a tibia fracture take to heal?
A straightforward fracture usually takes about 12 to 16 weeks. If the break is more serious and needs surgery, expect 4 to 6 months or more for a full recovery.
Can you walk with a fractured tibia?
Probably not right away. Most tibial fractures make weight-bearing extremely painful. In some cases, a stable fracture may let you walk with a brace or boot — but only if your doctor gives you the green light.
What’s the difference between the tibia and fibula?
The tibia is bigger and carries most of your body weight. The fibula is thinner, runs along the outer side, and mainly works as an anchor for muscles and a stabilizer for your ankle.
Are shin splints serious?
Most of the time, no. Rest and proper care clear them up. But if you keep ignoring the pain, it can turn into a stress fracture and that’s a bigger deal. See a doctor if rest doesn’t help after a week or two.
What are the growth plates of the tibia?
They’re strips of cartilage near the top and bottom of the tibia. These are the zones where the bone grows longer during childhood and the teen years. They close up and turn into solid bone somewhere between age 15 and 18.
How do doctors use the tibia in emergencies?
When they can’t start a regular IV, doctors insert a needle into the tibia’s bone marrow a technique called intraosseous access. It delivers fluids and medications straight into the bloodstream, almost as fast as a normal IV.
Final Thought
Your tibia does way more than you probably realized. It carries your weight, anchors your muscles, forms key joints, stores bone marrow, and can even serve as a lifeline during a medical emergency. Most of the time, it works quietly without any complaints. Take care of it stay active, eat well, listen to your body, and don’t brush off pain that sticks around. A little attention today saves you from a lot of trouble down the road.
