Pain Behind Knee: What It Is, Causes, Treatment & Relief
That dull ache tucked right behind your knee. The tight pull you feel when you straighten your leg after sitting too long.
The swelling that shows up after a weekend hike and refuses to leave. Pain behind the knee is one of those complaints that almost everyone runs into at some point.
It can come from something as simple as tight hamstrings or something as serious as a blood clot.
The tricky part is that the back of your knee (doctors call it the posterior knee) is a busy little neighborhood. Tendons, ligaments, nerves, blood vessels, and a cushion of fat all share a small space called the popliteal fossa.
When any one of them gets irritated, the whole area complains.
This guide walks you through what’s really going on back there, what’s likely causing the pain, when it’s safe to wait it out, when you should drop everything and call a doctor, and what actually helps.
What Pain Behind the Knee
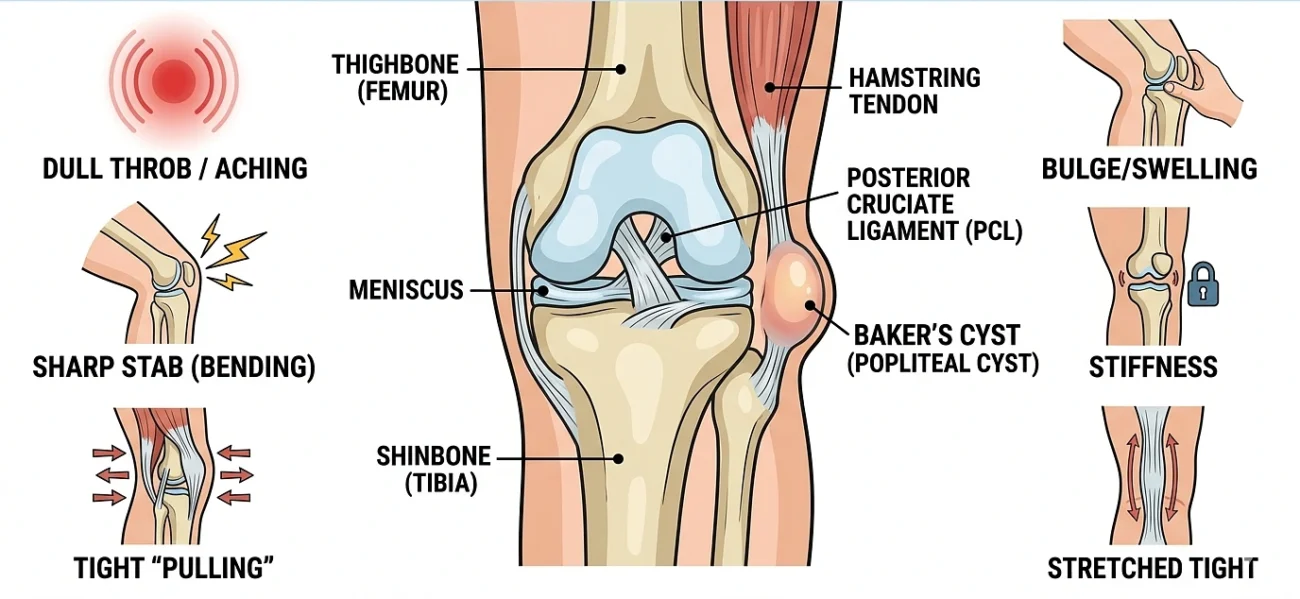
Pain behind the knee isn’t one feeling. It can show up as a dull throb, a sharp stab when you bend your leg, a tight “pulling” sensation, or a bulge you can actually feel if you press on the back of your knee.
Posterior knee pain may feel aching, stiff, sharp, or like something is stretched too tight. It often comes and goes depending on whether you’re moving or resting.
The knee joint itself is formed by three bones the thighbone (femur), shinbone (tibia), and kneecap (patella) held together by ligaments, tendons, and two wedge-shaped pieces of cartilage called the menisci.
Common Causes of Pain Behind the Knee
1. Baker’s Cyst (Popliteal Cyst)
If you can feel a soft, squishy bump behind your knee almost like a small water balloon you’re probably dealing with a Baker’s cyst.
It forms when the joint produces too much synovial (lubricating) fluid. That fluid then leaks out the back of the joint through a one-way valve and pools in the popliteal space, as explained.
Describes it as a fluid-filled cyst that develops behind the knee, often triggered by an underlying problem like arthritis or a cartilage tear.
It might cause no symptoms at all. Or you might notice stiffness, tightness when bending the knee, and swelling that gets worse after activity.
One important note: a PMC/NIH review of Baker’s cysts found that in a population of 399 patients with knee pain, popliteal cysts were present in about 26% of cases,.
Most Baker’s cysts settle down on their own. For stubborn ones, doctors may drain the fluid, inject a corticosteroid, or treat the underlying joint problem.
2. Hamstring Strain or Tendonitis
Your hamstring is actually a group of three muscles biceps femoris, semitendinosus, and semimembranosus that run down the back of your thigh and attach near the back of the knee.
When you over-sprint, over-stretch, or simply ask too much of them on a weekend run, the tendons near the knee can get irritated or torn.
Explains that a hamstring strain can range from a mild pull to a complete tear. Most respond well to rest, ice, compression, and elevation along with physical therapy.
Points out that hamstring tendonitis typically shows up as a dull ache at the back of the thigh, knee, or lower leg, along with stiffness when you walk or bend the knee.
3. Meniscus Tear
The menisci are two C-shaped pieces of cartilage that act as shock absorbers between your thighbone and shinbone.
A sudden twist stepping off a curb awkwardly, pivoting in a game of football, even standing up from a deep squat can tear them.
Explains that if you’ve torn your meniscus, it might take a day or more for pain and swelling to build up.
You may notice a popping sensation, stiffness, difficulty straightening the leg fully, or the feeling that your knee is “locked.”
Tears toward the back of the meniscus specifically cause pain that feels like it’s coming from behind the knee.
Treatment depends on the tear’s size and location. Small tears in the well-supplied outer rim may heal with rest and physical therapy. Larger or mechanical tears may need arthroscopic surgery, as Hospital for Special Surgery notes.
4. Posterior Cruciate Ligament (PCL) Injury
The PCL runs along the back of the knee and keeps your shinbone from sliding backward. It’s the strongest ligament in the knee.
It usually takes real force to injure it a hard fall onto a bent knee, a dashboard hit in a car accident, or an awkward landing during sport.
AAOS OrthoInfo notes that PCL injuries make up fewer than 20% of all knee ligament injuries.
Classic symptoms include pain that develops steadily, swelling that makes the knee stiff, and trouble walking.
A PCL tear rarely produces the loud “pop” people associate with an ACL tear. The pain tends to be deep, dull, and hard to pinpoint.
5. Knee Osteoarthritis
The wear-and-tear kind of arthritis is a huge contributor to knee pain, including pain behind the knee.
According to the U.S. CDC, osteoarthritis affects more than 32.5 million U.S. adults and most commonly strikes the hands, hips, and knees.
A systematic review by Cui et al. published in eClinicalMedicine (The Lancet), 2020 estimated the global prevalence of knee osteoarthritis at around 16% in people aged 15 and over, and roughly 22.9% in those aged 40 and over.
That’s close to 654 million adults worldwide living with it.
When cartilage thins inside the joint, the knee can swell, stiffen, and produce extra fluid that pushes toward the back of the knee. That’s exactly why arthritis is such a common trigger for Baker’s cysts.
6. Calf or Gastrocnemius Muscle Strain
The gastrocnemius is the big bulging muscle of your calf but its two heads actually attach above the knee joint.
A strain in the medial (inner) head of this muscle produces sharp pain at the back of the knee and upper calf.
It’s common enough in recreational athletes to have its own nickname: “tennis leg.” You’ll usually feel it as a sudden snap or pop, followed by swelling and difficulty pushing off the foot.
7. Deep Vein Thrombosis (DVT) A Medical Emergency
This is the cause you cannot ignore.
A deep vein thrombosis is a blood clot that forms in one of the deep veins of the leg. When the clot forms in the popliteal vein (which runs behind the knee), it’s called popliteal vein thrombosis.
The clot can break free and travel to the lungs, causing a life-threatening pulmonary embolism.
The risk factors are worth knowing. Being over 60, long periods of sitting (such as long flights or bed rest after surgery), pregnancy, hormonal birth control, smoking, obesity, and a personal or family history of clotting disorders all raise the odds.
If your pain behind the knee is paired with calf swelling, warmth, redness, or shortness of breath, treat it as an emergency. Do not stretch, massage, or “walk it off.”
Treatment & Relief Options
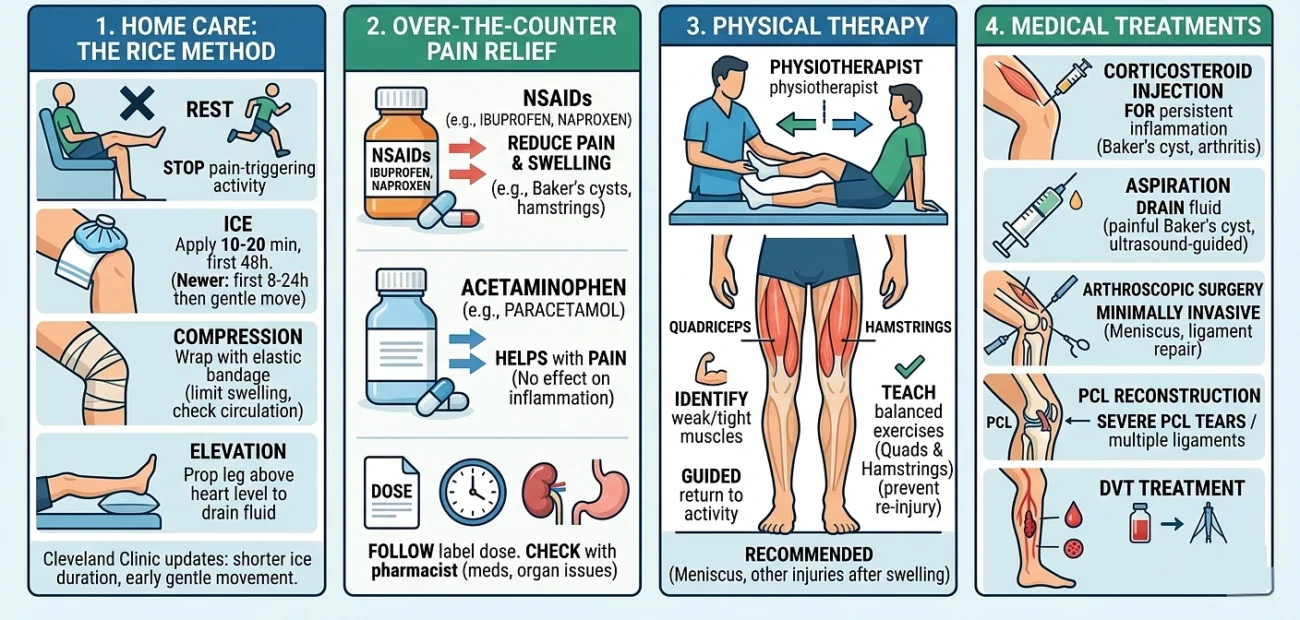
Home Care: The RICE Method
For most minor strains, sprains, and flare-ups, the first line of treatment is RICE Rest, Ice, Compression, Elevation.
Cleveland Clinic still recommends the approach for acute injuries, with a few modern tweaks:
- Rest – Stop any activity that triggers pain. You don’t need total bed rest; just avoid what hurts.
- Ice – Apply an ice pack wrapped in a towel for 10 to 20 minutes at a time, every one to two hours during the first 48 hours. Never put ice directly on skin.
- Compression – Wrap the knee with an elastic bandage to limit swelling. Loose enough that you’re not cutting off circulation.
- Elevation – Prop the leg above heart level when you’re sitting or lying down to help fluid drain.
Cleveland Clinic also points out newer thinking: keep ice to the first 8–24 hours, and start gentle movement soon after to avoid stiffness. Some clinicians now use updated acronyms like PEACE & LOVE to emphasize this.
Over the Counter Pain Relief
NSAIDs like ibuprofen and naproxen can reduce both pain and swelling. Recommends them as a first-line option for Baker’s cysts and hamstring injuries.
Acetaminophen (paracetamol) helps with pain but won’t touch inflammation.
Always stay within the dose on the label. Check with a pharmacist if you take other medications or have kidney, liver, or stomach issues.
Physical Therapy
This is where a lot of the long-term recovery happens.
A physiotherapist can identify weak or tight muscles, teach you exercises that strengthen the quadriceps and hamstrings in balance, and guide you back to activity in a way that doesn’t re-injure the area.
The recommends physiotherapy for meniscus tears and many other knee injuries once the initial swelling has calmed down.
Strong, flexible hamstrings and quads protect the knee from the inside out. Don’t skip this step just because the pain has started to fade.
Medical Treatments
If conservative care isn’t enough, your doctor may recommend:
- Corticosteroid injection – for persistent inflammation, particularly with Baker’s cysts or arthritis flares.
- Aspiration – draining fluid from a large, painful Baker’s cyst, sometimes guided by ultrasound.
- Arthroscopic surgery – a minimally invasive procedure used for many meniscus tears and for repairing severe ligament injuries.
- PCL reconstruction – typically reserved for severe PCL tears with instability or injuries involving multiple ligaments.
For DVT, treatment is very different – anticoagulant (blood-thinning) medications, and sometimes a filter placed in the vena cava to catch traveling clots.
This is managed by a physician, not at home.
When to See a Doctor
Cleveland Clinic recommends seeing a healthcare provider if pain behind the knee lasts more than a few days or keeps you from your normal activities.
Beyond that, there are red-flag symptoms that mean now, not later:
- Sudden, severe calf or knee swelling on one side only.
- Warmth, redness, or discoloration of the calf.
- Shortness of breath, chest pain, or coughing up blood (possible pulmonary embolism).
- A knee that looks deformed or won’t bear any weight.
- Fever with a hot, red, painful knee (possible joint infection).
- A loud pop at the moment of injury, followed by rapid swelling.
For anything in that list, skip the online symptom checkers and get to an emergency room.
References
- Mass General Brigham – Hamstring Injuries: https://www.massgeneralbrigham.org/en/patient-care/services-and-specialties/sports-medicine/conditions/knee/hamstring-injuries
- Merck Manual (Professional) – Baker Cysts: https://www.merckmanuals.com/professional/musculoskeletal-and-connective-tissue-disorders/bursa-muscle-and-tendon-disorders/baker-cysts
- CDC – Osteoarthritis: https://archive.cdc.gov/www_cdc_gov/arthritis/types/osteoarthritis.htm
- Cui A. et al., “Global, regional prevalence, incidence and risk factors of knee osteoarthritis in population-based studies,” eClinicalMedicine (The Lancet), 2020: https://www.thelancet.com/journals/eclinm/article/PIIS2589-5370(20)30331-X/fulltext
- Baker’s Cyst – PMC/NIH review: https://pmc.ncbi.nlm.nih.gov/articles/PMC8754354/
- Ruptured Baker’s Cyst Review – PMC: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC12810733/
