Cardiac Arrest: Signs, Symptoms, Treatment
Overview
Cardiac arrest is one of those life-threatening emergencies where time is of the essence. It’s the heart stopping, the person falling and without immediate treatment, they’re dead. It’s often confused for a heart attack, but it isn’t. A heart attack is when there’s a lack of blood to the heart. Sudden cardiac arrest is when the heart stops. A heart attack is a circulation problem. Sudden cardiac arrest is an electrical problem.
It’s not just a naming convention it matters. And if you’re in the US there’s a pretty good chance you’ll witness one of approximately 350,000 out-of-hospital cardiac arrests that occur each year.
What’s is Cardiac Arrest
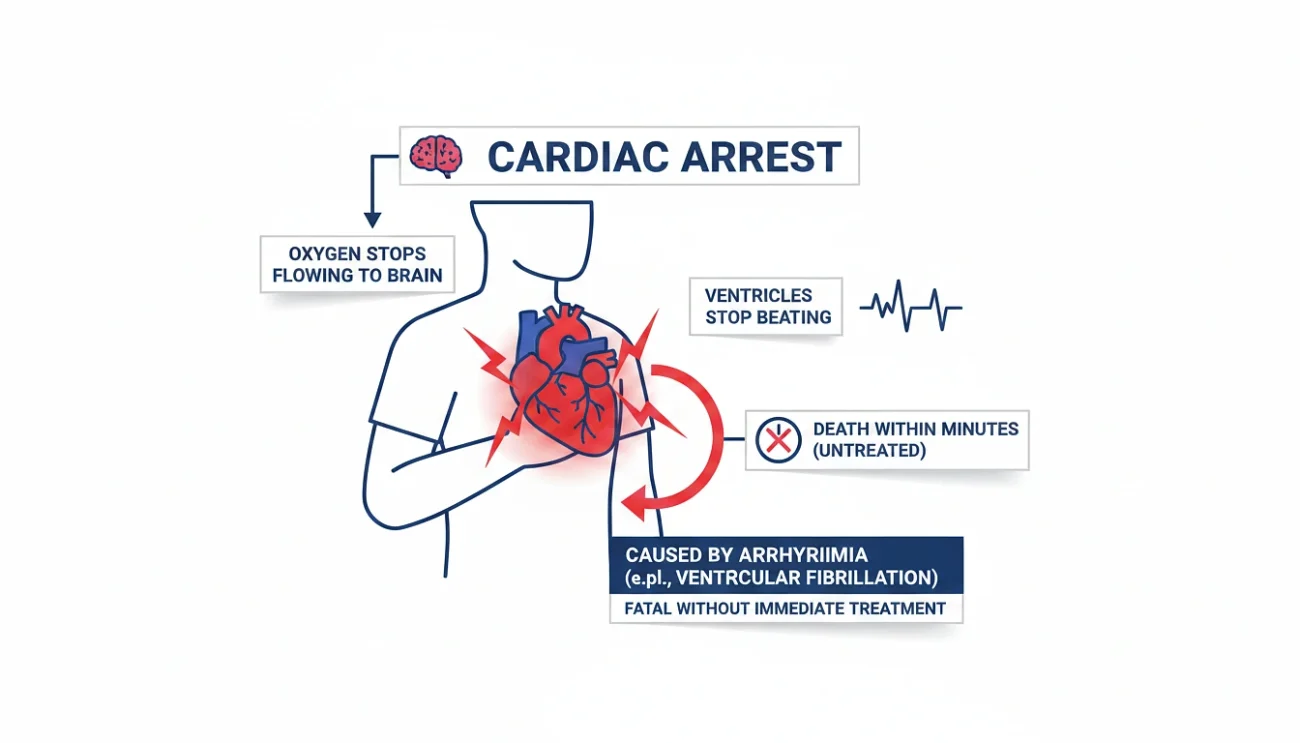
It’s like the electrical system in the heart short-circuits. The ventricles stop beating and oxygen stops flowing to the organs, and in particular the brain, which consumes oxygen at a rate far faster than anything else, begins to die very quickly. Untreated, cardiac arrest results in death within a few minutes. If it’s treated in the first few minutes of occurrence, cardiac arrest can be reversed on occasion.
Most of the time, an arrhythmia kicks the whole thing off, and ventricular fibrillation is the usual culprit. VF has been identified in nearly 70% of cardiac arrest patients. Without treatment, the condition is fatal within minutes.
Signs and Symptoms of Cardiac Arrest
The bad news is cardiac arrest can come out of the blue. Around 50 percent of people don’t have any symptoms before their cardiac arrest. The remaining 50 percent may feel out of sorts in the hour leading up to, or even weeks later.
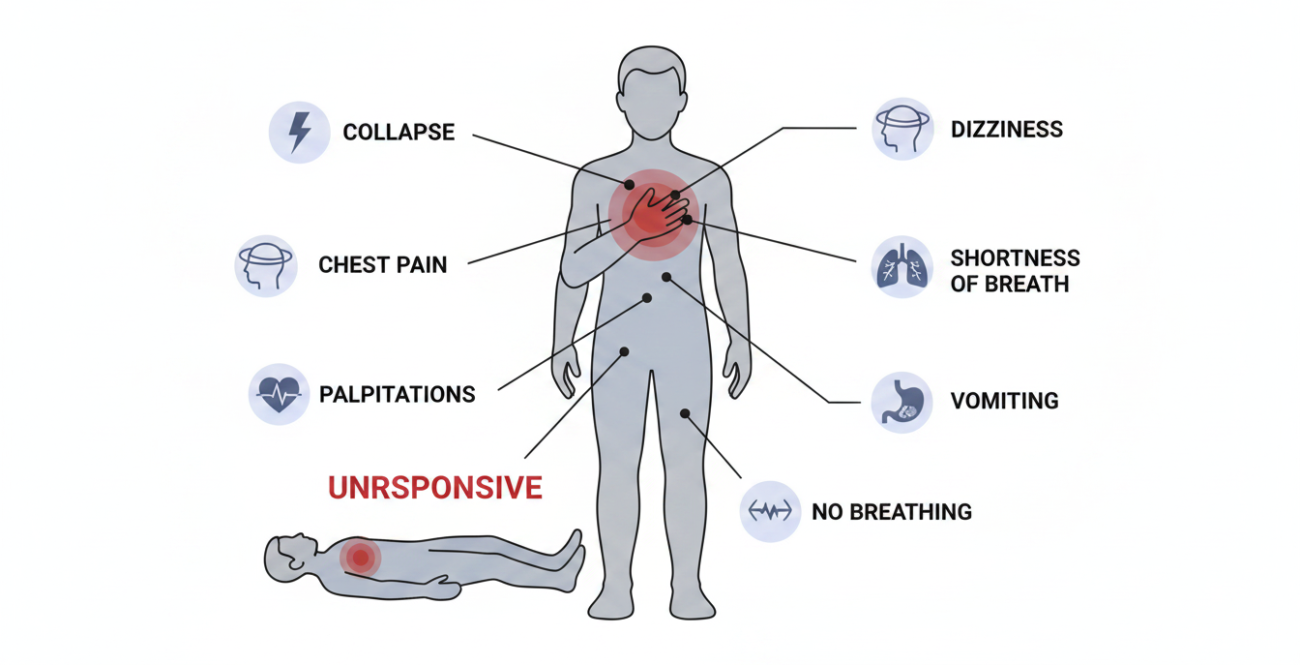
The signs are obvious and they happen fast:
- A sudden collapse – no warning, they just go down
- No response at all – the person doesn’t respond, even if you tap them hard on the shoulders. The person doesn’t move, speak, blink or otherwise react.
- No real breathing – either nothing, or strange gasping. That gasping has a name (agonal breathing) and it’s not actual breathing, so don’t let it fool you
Lots of people get nothing, but when warning signs do occur, they’re not to be ignored. There are sometimes warning signs before sudden cardiac arrest that include feeling weak or even passing out, dizziness, chest pain, shortness of breath, palpitations or vomiting.
And it pays to do something about them: People who seek medical care for warning signs are 5 times more likely to survive cardiac arrest. In other words, passing out, odd chest pain, unexplained palpitations? Don’t shrug them off.
What to Do Right Now The Three Things
If you’re ever the bystander, this is your whole job. The window is small and what happens in the first few minutes matters more than anything that comes later in a hospital.
1. Call for help
In the US, 911. Different country, different number just call. If two people are around, one calls while the other starts CPR. Alone? Call first, then start.
2. Start CPR push hard, push fast
This is the single biggest thing a bystander can do. If performed immediately, CPR can double or triple the chance of survival from an out of hospital cardiac arrest.
- Heel of one hand in the center of the chest, the other hand on top.
- Press down at least 2 inches (around 5 cm)..
- 100 to 120 compressions a minute.
- Let the chest spring all the way back between pushes.
- Keep going until help shows up or an AED is ready.
In adult victims of cardiac arrest, it is reasonable for rescuers to perform chest compressions at a rate of 100 to 120/min and to a depth of at least 2 inches (5 cm) for an average adult, while avoiding excessive chest compression depths (greater than 2.4 inches [6 cm]).
If rescue breaths feel out of your league, skip them. Hands-only CPR works fine. For the general public or bystanders who witness an adult suddenly collapse: compression-only CPR, or Hands-Only CPR. Hands-Only CPR is CPR without mouth-to-mouth breaths.
A weirdly useful trick: songs in the 100–120 BPM range make great metronomes. “Stayin’ Alive” is the classic a little dark, but it does the job.
3. Grab an AED if there’s one nearby
An Automated External Defibrillator is designed for laymen. You plug it in, follow the voice prompts and off you go. It will only shock if needed, there’s no way to shock someone who doesn’t need it.
Why the rush? Defibrillation within the first minute has been reported to have a survival rate of up to 90%. If defibrillation is delayed the survival rate drops to approximately 50% at 5 minutes, approximately 30% at 7 minutes, approximately 10% at 9 to 11 minutes and approximately 2% to 5% at 12 minutes or more.
Long-Term Treatment for Survivors
Once someone makes it through the initial event, the hospital phase has two goals figure out what caused it, and stop it from happening again.
Implantable Cardioverter-Defibrillator (ICD)
For many survivors, this is the key. It’s a little device that’s implanted into the body and continuously monitors the heart’s rhythm. If it notices something bad, it will give your heart a shock automatically it’s like having an AED in your chest.
ICDs cut the rate of sudden cardiac death by 50% compared to amiodarone. ICDs are currently recommended for secondary prevention in patients with documented VF or hemodynamically unstable VT and in the absence of reversible causes.
Medications
The drugs attack different targets: beta-blockers calm down the electrical pacing of the heart, antiarrhythmics prevent the dangerous rhythms from starting, ACE inhibitors and statins target the underlying problems of the heart’s blood vessels. The combination varies, depending on the original cause for the arrest.
Procedures to fix the root cause
If a blocked artery was behind it (and it often is), procedures like angioplasty, stenting, or bypass surgery may be needed to open things back up and head off another event.
Genetic testing for the family
This part’s often forgotten. You and your blood relatives may be offered genetic testing. This is because some of the things that can put you at risk of cardiac arrest are genetic. If your condition was genetic, your brothers and sisters and your children may be at risk and it’s important they know.
What’s Behind It
The heart is basically an electrical pump, and cardiac arrest is what happens when the electrical side fails. Arrhythmias are usually what triggers it ventricular fibrillation most often but those arrhythmias don’t appear out of thin air. Something underneath is usually setting them off.
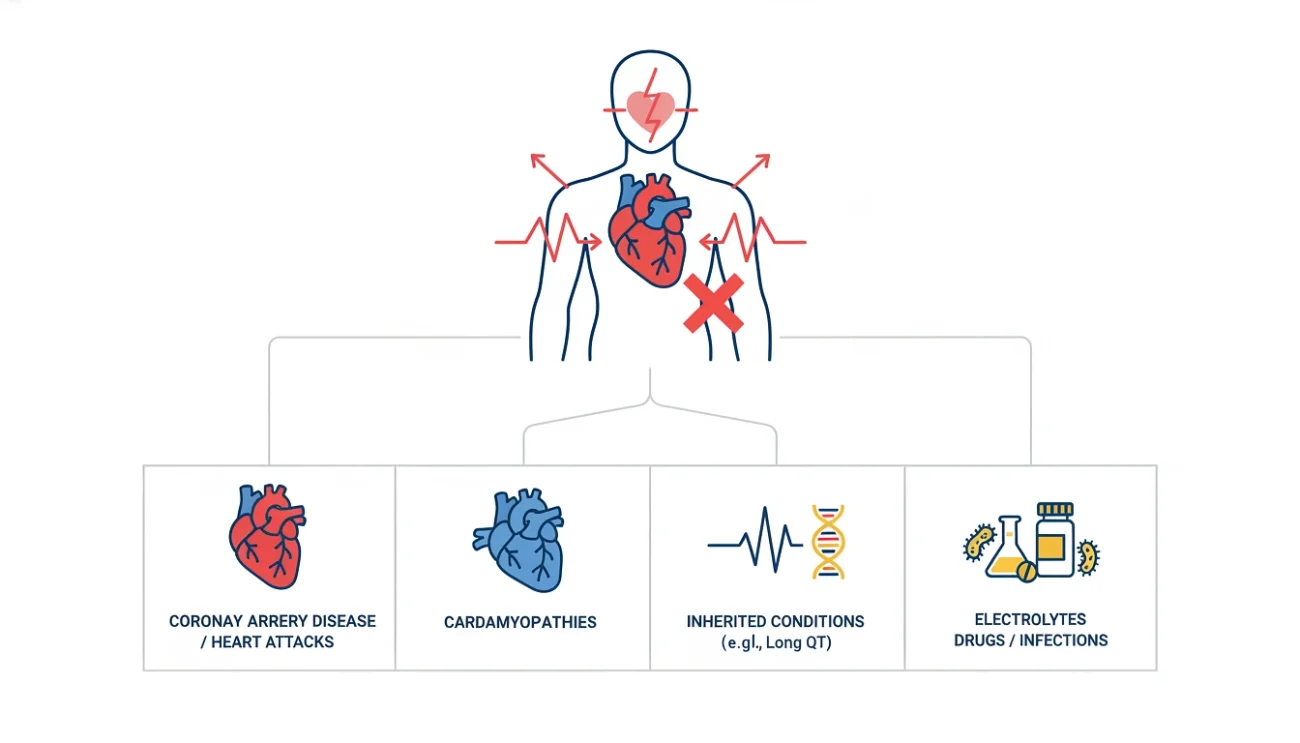
The common culprits:
- Coronary artery disease and heart attacks by far the biggest. The most common cause of ventricular fibrillation is a heart disorder, particularly inadequate blood flow to the heart muscle due to coronary artery disease, as occurs during a heart attack.
- Cardiomyopathies diseases of the heart muscle itself
- Inherited heart conditions long QT syndrome, Brugada syndrome, hypertrophic cardiomyopathy. Long QT syndrome alone shows up in roughly 1 in 2,500 live births, and it can stay quiet for years until it suddenly isn’t.
- Electrolyte problems, drug toxicity, and serious infections can all set off fatal arrhythmias too
