10 Root Causes of Fibromyalgia: What’s Really Behind Your Pain

Every day, millions of people wake up exhausted not from a bad night's sleep, but from a relentless, full-body pain that no scan can find and no simple medication can fix. They are told, far too often, that the pain is "all in their head." It is not.Fibromyalgia (FM) is a real, complex, and life-altering chronic condition. It affects an estimated 2–4% of the global population, with women diagnosed at roughly ten times the rate of men.
Despite decades of research, it remains one of medicine’s most misunderstood syndromes partly because it wears so many faces, and partly because its roots run deeper than a single system in the body.
Understanding why the pain exists is the first step toward reclaiming your life.
What Is Fibromyalgia?
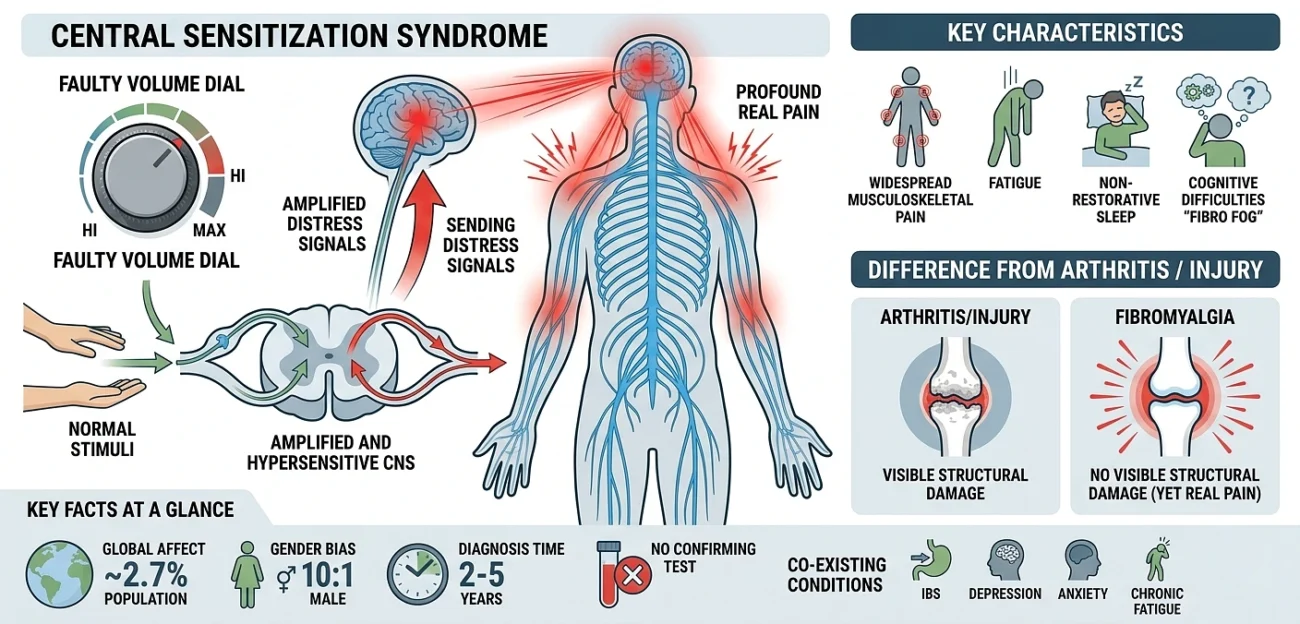
Fibromyalgia is a chronic pain syndrome primarily characterized by widespread musculoskeletal pain, fatigue, non-restorative sleep, and cognitive difficulties often called “fibro fog.”
Unlike arthritis or a physical injury, fibromyalgia produces no visible structural damage to joints, muscles, or nerves yet the pain is profoundly real.
Current science classifies it as a central sensitization syndrome: a condition where the central nervous system becomes amplified and hypersensitive, sending distress signals in response to stimuli that would not normally cause pain. Think of it as a faulty volume dial the pain system is turned up too high and cannot come back down.
Key facts at a glance:
- Affects approximately 2.7% of the world population.
- Female-to-male diagnosis ratio: approximately 10:1.
- Average time to correct diagnosis: 2–5 years.
- No single blood test or imaging scan can confirm it.
- Frequently co-exists with IBS, depression, anxiety, chronic fatigue syndrome, and autoimmune diseases.
Why Identifying the 10 Root Causes of Fibromyalgia
For years, fibromyalgia was dismissed or blamed entirely on psychological factors. The research of the past decade has shattered that view.
We now know fibromyalgia has multiple, intersecting biological roots and identifying them matters enormously:
- It validates patients. The pain is not imaginary. It has measurable biological mechanisms.
- It guides treatment. A person whose fibromyalgia is rooted in trauma needs different support than someone whose root cause is immune dysfunction.
- It opens new therapies. Discovering that gut bacteria can cause pain hypersensitivity opens the door to microbiome-based treatments.
- It prevents misdiagnosis. Understanding the full picture reduces years of unnecessary testing, wrong treatments, and emotional suffering.
Symptoms of Fibromyalgia
Before exploring the causes, it helps to understand the full symptom picture. Fibromyalgia is far more than widespread pain.
| Symptom | Symptom Description |
|---|---|
| Primary Symptoms | |
| Widespread musculoskeletal pain | Aching, burning, or stabbing sensations across the entire body. |
| Allodynia | Pain triggered by stimuli that should not cause pain (e.g., light touch, gentle pressure). |
| Hyperalgesia | Exaggerated pain from stimuli that normally cause only mild discomfort. |
| Secondary Symptoms | |
| Fatigue | Profound, unrelenting exhaustion, often described as “lead-heavy” limbs. |
| Non-restorative sleep | Waking after a full night’s rest still feeling completely exhausted. |
| Fibro fog | Difficulty with memory, concentration, word-finding, and mental clarity. |
| Morning stiffness | Joint and muscle stiffness, typically worst upon waking. |
| Frequent headaches/migraines | Persistent headaches and migraines. |
| Irritable Bowel Syndrome (IBS) | Bloating, cramping, alternating constipation and diarrhea. |
| Heightened sensitivity | Increased sensitivity to noise, light, temperature, and smell. |
| Anxiety and depression | Both very common co-occurring conditions. |
| Restless leg syndrome | Uncomfortable sensations in the legs, especially at night. |
| Numbness and tingling | Particularly in the hands and feet. |
| Temperature dysregulation | Intolerance to cold or heat. |
| Sexual dysfunction | Reduced libido and discomfort. |
Note: Symptoms vary widely between individuals and can fluctuate in “flares” periods of significantly worsened symptoms that may last days or weeks.
The 10 Root Causes of Fibromyalgia
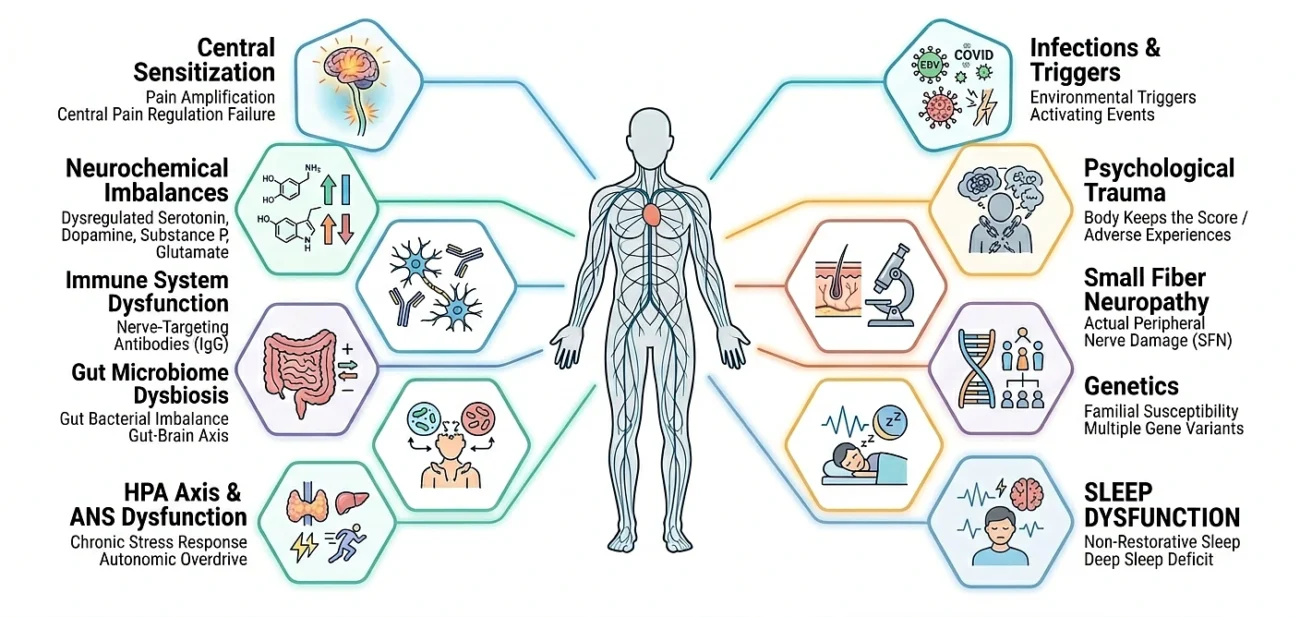
Central Sensitization
At the very core of fibromyalgia lies central sensitization: a state in which the central nervous system becomes abnormally amplified in how it processes pain.
In a healthy nervous system, pain is a signal. It alerts you to harm and once the threat is gone, the signal quiets down. In fibromyalgia, this “off switch” malfunctions. The nervous system stays on high alert, amplifying even mild or non-threatening stimuli into painful experiences.
What the research shows:
- MRI studies consistently reveal altered brain activity in fibromyalgia patients, with differences in regions responsible for pain processing
- The dorsal horn of the spinal cord a key pain relay station shows “wind-up,” where repeated stimuli produce increasingly intense responses
- Neuroimaging confirms fibromyalgia brains respond differently to pain compared to healthy individuals
Central sensitization is considered the defining mechanism of fibromyalgia. All other root causes, in many ways, feed into and amplify this phenomenon.
Neurochemical Imbalances
The brain depends on a precise balance of neurotransmitters (chemical messengers) to regulate pain, mood, and sleep. In fibromyalgia, several key systems are disrupted.
- Serotonin – helps dampen pain signals is consistently low in fibromyalgia patients. This is why antidepressants that boost serotonin are among the few FDA-approved treatments.
- Dopamine – essential for pain modulation and reward also shows significant dysregulation.
- Substance P – a neuropeptide that amplifies pain is found at levels roughly three times higher than in healthy individuals.
- Glutamate – an excitatory neurotransmitter over-activates nerve cells, contributing to the heightened pain state.
- Norepinephrine – involved in the stress response is dysregulated, driving autonomic symptoms.
These imbalances are not simply consequences of living in pain. Research suggests they are active contributors and genetic variants affecting serotonin transporters, dopamine receptors, and COMT enzymes have been identified as predisposing factors.
Immune System Dysfunction and Autoimmune Mechanisms
For decades, fibromyalgia was assumed to be a brain problem. Landmark research from King’s College London, the University of Liverpool, and the Karolinska Institute has dramatically changed this picture.
These studies demonstrated that many fibromyalgia symptoms are caused by IgG antibodies immune proteins that abnormally increase the activity of pain-sensing nerves throughout the body.
The breakthrough findings:
- When IgG antibodies from fibromyalgia patients were transferred into mice, the animals rapidly developed pain hypersensitivity, muscle weakness, and reduced movement mirroring human fibromyalgia precisely
- Neutrophils (white blood cells) from fibromyalgia patients invade neuron cell bodies outside the spinal cord behavior not seen with healthy donors’ cells.
- Levels of antibodies against satellite glia cells (nerve-supporting cells) correlated directly with symptom severity.
- Inflammatory proteins including TNF-α and IL-12β have been causally linked to fibromyalgia risk through genetic studies.
This evidence strongly suggests that fibromyalgia may be a disease of the immune system a finding that opens an entirely new field of therapeutic possibilities.
Gut Microbiome Dysbiosis
Your gut contains trillions of microorganisms that collectively regulate immunity, neurotransmitter production, inflammation, and pain perception. In fibromyalgia, this ecosystem is measurably disrupted.
The gut-brain axis the communication network linking the gut and brain via the vagus nerve, immune signals, and neurotransmitter pathways is now considered a pivotal mechanism in fibromyalgia.
HPA Axis and Autonomic Nervous System Dysfunction
The hypothalamic-pituitary-adrenal (HPA) axis is the body’s master stress-response system. When activated by stress, it triggers hormones — most notably cortisol — designed to mobilize the body for danger.
In fibromyalgia, this system is chronically dysregulated.
- Elevated hair cortisol concentrations a reliable marker of chronic stress have been confirmed in fibromyalgia patients
- Blood pressure regulation relies on increased vascular resistance, reflecting impaired autonomic flexibility
- The sympathetic nervous system (the “fight or flight” branch) appears hyperactive, driving symptoms like heart rate variability, excessive sweating, dizziness, and temperature intolerance
- Chronic HPA dysfunction perpetuates the cycle of neuroinflammation and central sensitization
In practical terms: the body of a fibromyalgia patient is perpetually stuck in a stress-response loop, unable to fully return to a state of rest and repair.
Small Fiber Neuropathy
One of the most significant recent discoveries is that many fibromyalgia patients have small fiber neuropathy (SFN) actual, measurable damage to the tiny nerve fibers responsible for transmitting pain, temperature, and autonomic signals.
The evidence is clear:
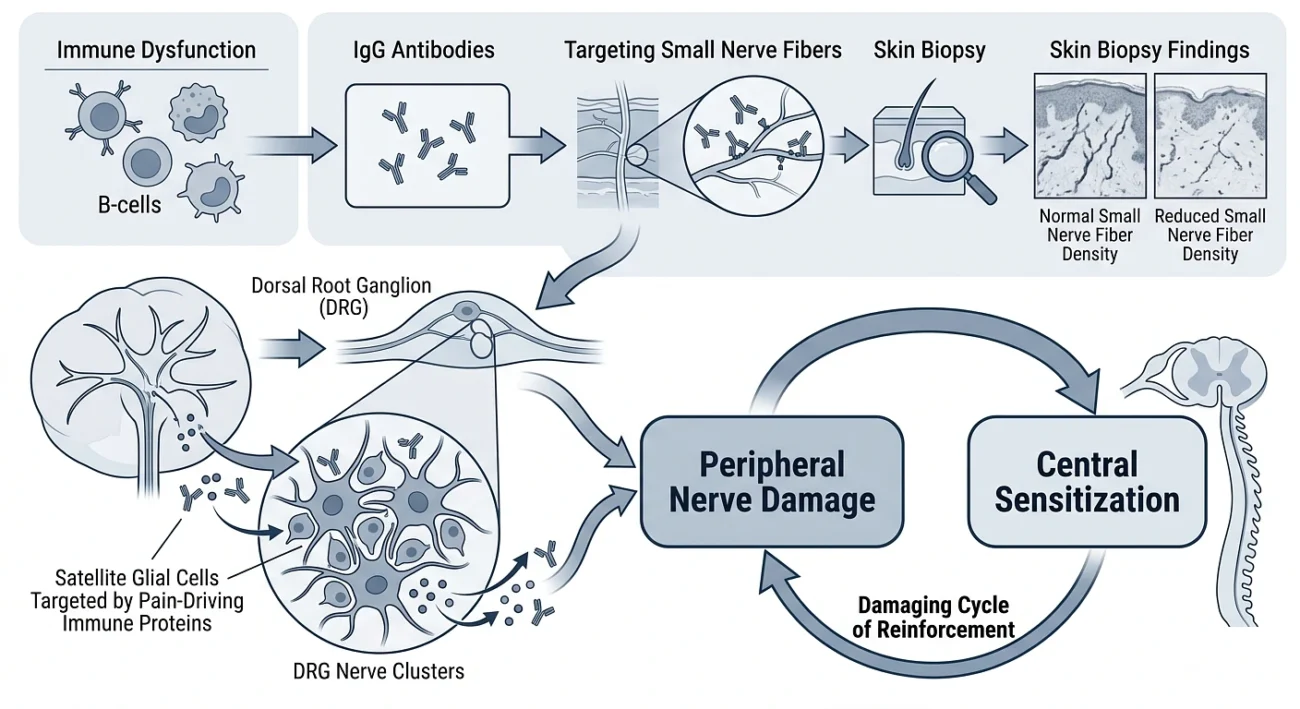
The recognition of small fiber neuropathy confirms that fibromyalgia is not purely a “brain” problem it involves real, measurable damage at the peripheral level too.
Genetic Predisposition It Can Run in the Family
Fibromyalgia is not caused by a single gene, but genetics clearly plays a predisposing role. People with a first-degree relative who has fibromyalgia are roughly 8 times more likely to develop it.
Key genetic findings:
- Variants in the serotonin transporter gene (SLC6A4) affect how efficiently the brain manages pain-moderating serotonin signals.
- Mutations in the COMT gene influence pain sensitivity and stress reactivity by affecting how the brain breaks down dopamine and norepinephrine.
- Variants in the dopamine D4 receptor gene (DRD4) impair the brain’s pain-modulation system.
- Genome-wide association studies (GWAS) continue to identify new genetic markers associated with FM risk.
Importantly, genetics alone rarely causes fibromyalgia. It creates a susceptibility that environmental triggers then activate explaining why some people develop fibromyalgia after a specific event while others with the same genes never do.
Psychological Trauma and Adverse Life Events
The relationship between trauma and fibromyalgia is neither simple nor reductive. Acknowledging it does not mean the condition is “psychological.” It means the body keeps the score.
Physical and emotional trauma can fundamentally rewire the nervous system’s pain architecture:
- Childhood adverse experiences (ACEs) including abuse, neglect, and household dysfunction are significantly overrepresented in fibromyalgia patients.
- Trauma dysregulates the HPA axis, rewires neural pain-processing pathways, and alters immune function in ways that can persist for decades.
- PTSD and fibromyalgia frequently co-occur, sharing overlapping neurobiological mechanisms.
- Physical trauma car accidents, surgeries, and serious illness can trigger fibromyalgia onset in genetically susceptible individuals.
Critically, research has confirmed that depression does not cause fibromyalgia. When fibromyalgia-like symptoms were induced in mice via gut microbiome transfer, depression emerged months later confirming that psychological distress is most often a consequence, not a cause.
Sleep Dysfunction The Restorative Failure Loop
Non-restorative sleep is both a hallmark symptom and an active root cause of fibromyalgia creating a damaging, self-reinforcing feedback loop.
- Disrupting slow-wave (deep) sleep in healthy volunteers can produce widespread musculoskeletal pain and tenderness within just a few days pain that resolves once normal sleep is restored.
- In fibromyalgia, disruptions to delta (stage 3) sleep are widespread, meaning the body never fully enters the restorative phase where cellular repair and pain modulation occur.
- Poor sleep independently increases inflammatory cytokines, lowers pain thresholds, and impairs the body’s natural pain-inhibitory systems.
- Alpha wave intrusions into deep sleep abnormal brain wave patterns common in fibromyalgia disrupt restorative sleep quality even when sleep quantity appears sufficient.
The relationship is bidirectional and relentless: pain disrupts sleep, and disrupted sleep amplifies pain making targeted sleep intervention one of the most important steps in fibromyalgia management.
Infections, Physical Stressors, and Environmental Triggers
For many fibromyalgia patients, the condition has a clear starting point: a viral illness, a physical injury, or a period of intense stress. These act as triggers in people who carry the underlying biological susceptibilities described above.
Established and emerging triggers include:
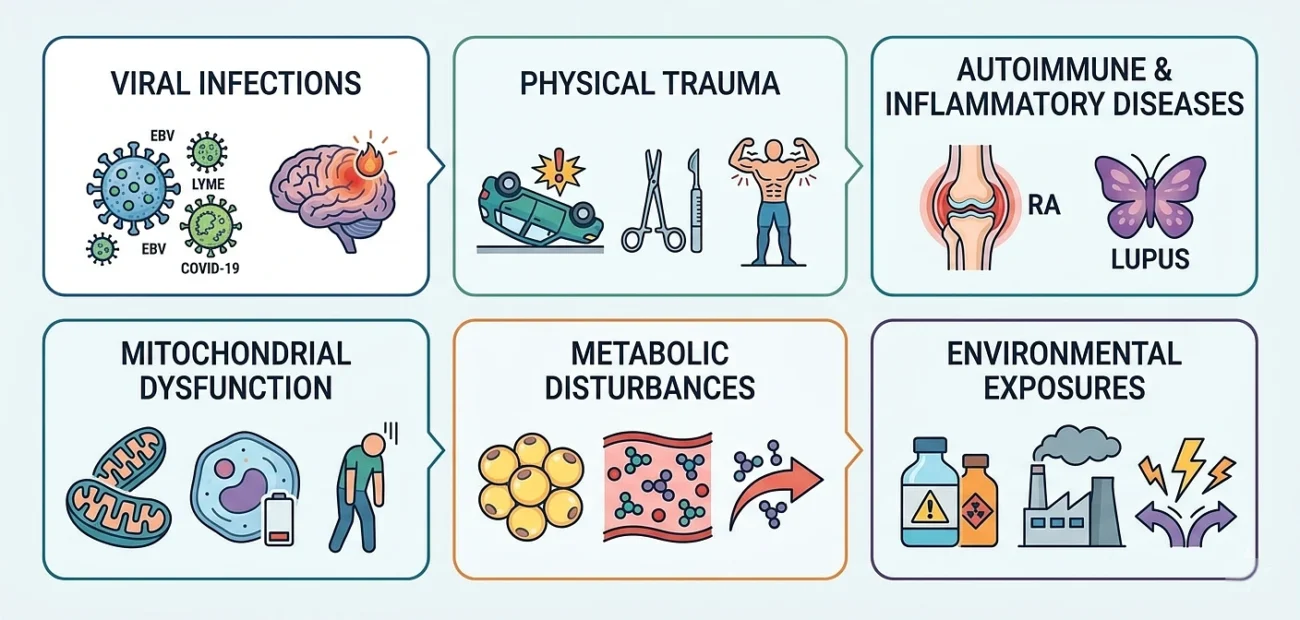
References & Key Sources
- Iannuccelli C, et al. Fibromyalgia: One Year in Review 2025. Clin Exp Rheumatol. 2025;43(6):957–969.
- Di Carlo M, et al. Fibromyalgia: One Year in Review 2024. Clin Exp Rheumatol. 2024;42(6):1141–1149.
- Caxaria S, Sikandar S, et al. Is Fibromyalgia an Autoimmune Disease? PNAS. 2023;120(17).
- Minerbi A, Khoutorsky A, Shir Y. Decoding the Connection: Unraveling the Role of Gut Microbiome in Fibromyalgia. Pain Reports. 2025;10(1).
- Palma-Ordóñez et al. Implication of Intestinal Microbiota in the Etiopathogenesis of Fibromyalgia. Int J Rheumatic Diseases. 2024.
- King’s College London. New Study Shows Fibromyalgia Likely the Result of Autoimmune Problems. 2021.
- American Fibromyalgia Syndrome Association (AFSA). Research Update 2024–2025.
- Scientific Reports. Exploring Gut Microbiota Alterations and Their Associations with Clinical Symptoms in Fibromyalgia. 2025.
- PMC. Decoding Fibromyalgia: Genetic Insights into Gut and Immune System Interactions. J Pain Res. 2025.
